 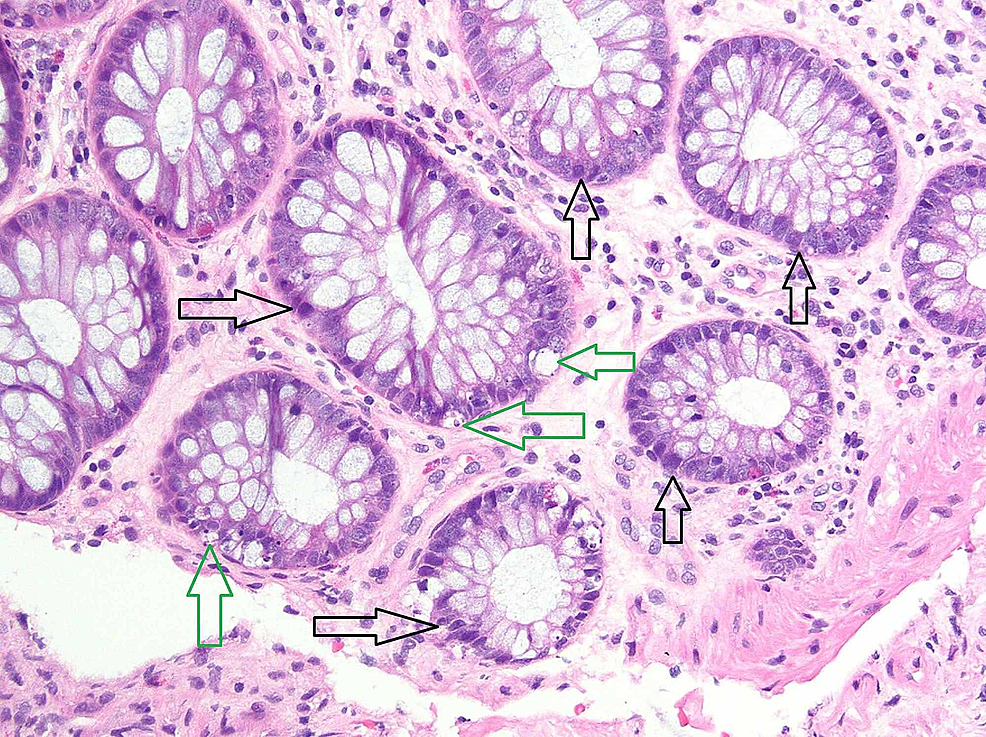
Inflammation is limited to the mucosa and submucosa.Ascending inflammationthat begins in the rectum and spreads continuously proximally throughout the colon.Autoantibodies ( pANCA) against cells of the intestinal epithelium.Dysregulation of the immune system: upregulation of lymphatic cell activity ( T cells, B cells, plasma cells) in bowel walls → enhanced immune reaction and cytotoxic effect on colonic epithelium → inflammation with local tissue damage (ulcerations, erosions, necrosis) in the submucosa and mucosa.Differentiation of naive CD4+ cells to Th2 effector cells.Secretion of proinflammatory cytokines ( IL-6, IL-12, TNF-α) and chemokines (CXCL1, CXC元, and CXCL8) → recruitment of other immune cells (e.g., neutrophils) to the site.Dysregulation of intestinal epithelium: increased permeability for luminal bacteria → activation of macrophages and dendritic cells → antigen presentation to macrophages and naive CD4+ cells leads to:.The exact mechanism is unknown but studies suggest that ulcerative colitis is caused by abnormal interactions between host immune cells and commensal bacteria. Remission criteria (ACG): no diarrhea, no visible blood in stools, no fecal urgency, fecal calprotectin Other: response to medication, disease course, and the patient's quality of life.American College of Gastroenterology (ACG) ulcerative colitis activity index.Mayo score for ulcerative colitis activity.A combination of both endoscopic findings and clinical presentation.Truelove and Witts severity index for ulcerative colitis.Simple clinical colitis activity index (SCCAI).Ulcerative colitis endoscopic index of severity (UCEIS).There are several classification systems that can be used to assess disease severity. Limited to the colon distal to the splenic flexureĬlassification of ulcerative colitis by severity 
Montreal classification for the extent of ulcerative colitis Patients with ulcerative colitis are at increased risk of developing colorectal cancer and should undergo regular endoscopic surveillance. Proctocolectomy is curative and indicated in patients with complicated ulcerative colitis or dysplasia. In distal colitis, medications may be administered rectally (e.g., via enema), whereas more proximal inflammation requires oral treatment. Patients who experience severe episodes often require corticosteroids or other immunosuppressants to achieve remission. 5-Aminosalicylic acids (e.g., mesalamine) are the mainstay of treatment for mild-to-moderate disease. Definitive diagnosis requires endoscopy, which may show changes to superficial vascular patterns, friable mucosa, and erosions and/or ulcerations. Although not required for diagnosis, the presence of perinuclear antineutrophil cytoplasmic autoantibodies ( pANCA) is suggestive of ulcerative colitis. Laboratory findings typically show elevated inflammatory markers (e.g., ESR, CRP) and elevated fecal calprotectin. Common symptoms include bloody diarrhea, abdominal pain, and fecal urgency. Ulcerative colitis is an inflammatory bowel disease ( IBD) characterized by chronic mucosal inflammation of the rectum, colon, and cecum. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
